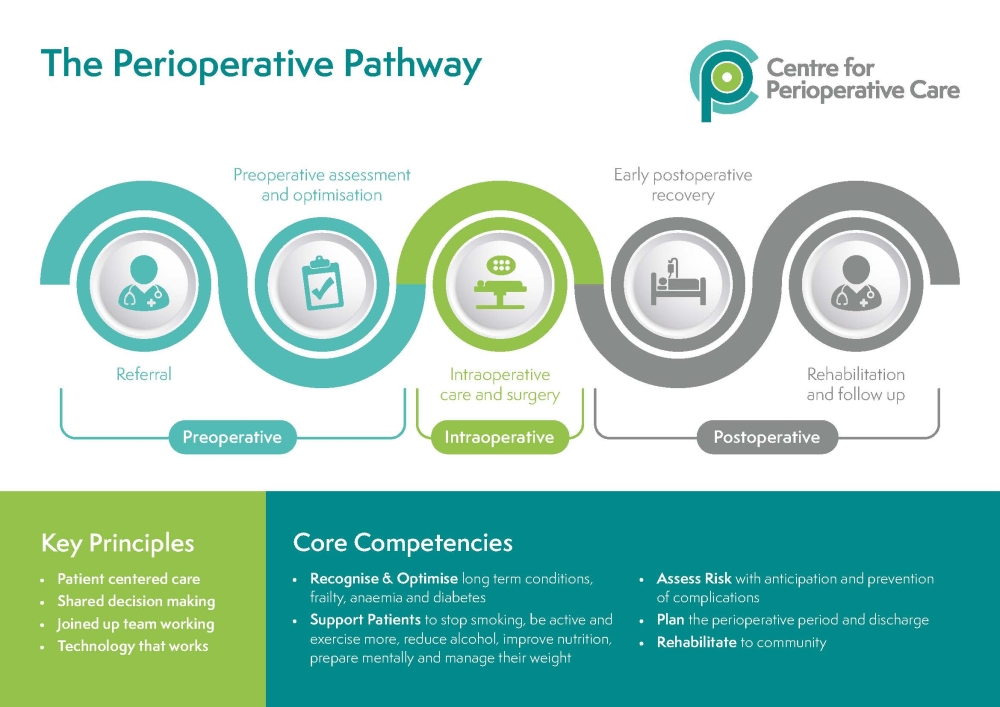
CPOC Strategy 2023-2026
CPOC is dedicated to the advancement of perioperative care through focusing on five main strategic themes identified by the CPOC Board
Our Strategy for the Centre for Perioperative Care (CPOC) 2023-2026 highlights our vision, who we are, our values and strategic aims.
Our Vision
To improve the health of people of all ages, at all stages of their surgical journey, by promoting the highest standards of perioperative care.
Our Values
- Patient focussed
- Multi-professional and Collaborative
- Proactive and Committed
- Diverse and Inclusive
- Forward thinking and Ambitious
What we will do and our strategic priorities
Our goal is to implement perioperative care pathways across geographical partnerships of healthcare providers and commissioners, local authorities and other partners who work together to plan and integrate care. This will enable providers to work collaboratively to deliver seamless patient care and long-term population health benefits, realising every opportunity to improve patient health.
Our objective is to embed prevention, including perioperative care pathways into routine clinical practice.
We will lead the development of a suite of guidelines with the aim of setting and improving standards of clinical practice. The CPOC Board will identify relevant topics that align with our strategic goals such as the needs of patients undergoing day case surgery.
It is our aim to:
- develop relevant guidelines
- share good practice and innovation (case studies, vignettes)
- facilitate dissemination of data (via national programmes including Getting it Right First Time (GIRFT) 8 and Perioperative Quality Improvement program (PQIP))
- support quality improvement through education and training, to develop resources for trainees that will increase both knowledge and interest in perioperative care leading to improved outcomes
- collate resources and ensure accessibility across the NHS
CPOC seeks to improve shared decision-making and personalised care for patients: changing the rhetoric so patient empowerment is seen as fundamental to every health interaction. CPOC will create and signpost clear patient information. Our resources will address:
- exercise, nutrition, obesity and smoking
- psychological support
- long term conditions management such as pain management and opioids before surgery
- shared decision-making resources for patients and carers
Delivering quality perioperative care requires a workforce equipped to manage patients in different healthcare settings and undergoing all types of surgery from minor to complex procedures. CPOC recognises the need for better use of the entire workforce through broader training, cross-skilling and a more flexible approach. Registered staff and students benefit from training in different aspects of perioperative care, shared decision making and motivational interviewing. It also requires a workforce that has good mental health and wellbeing.
CPOC will be a leader in perioperative education and we aim to educate all staff (including administrative and non-registered clinical staff) in the fundamentals of patient empowerment and perioperative care through education with clear identification of complexities and of patients who will need senior input. This builds on the NHS as an anchor institution, which refers to a large typically non-profit organisation whose long-term sustainability is tied to the wellbeing of the populations they serve. Building genuine teamwork, so everyone has a remit to take action, rather than just write it down, is the goal and good team-working is a key means of keeping staff engaged, empowered and motivated.7,8
CPOC will work with other organisations and Royal Colleges on educational initiatives and will be active on educational forums. We will work with partners and stakeholders to ensure perioperative care is included in relevant medical curriculum and guidance. We will collate, host and recommend quality assured resources and educational materials.
We aim to:
- develop a multi-professional curriculum in perioperative care that will form the basis of a credential training programme for post-CCT Doctors and allied health professionals
- foster and support the wellbeing of the perioperative workforce
- be the voice of the perioperative community
- collaborate with others to promote education of the workforce
CPOC is aiming to move to a new model of care from tradition silo and speciality working to collaborative, cross speciality pathway working. We will influence policy to embed perioperative care in health systems in the UK and beyond. This will involve:
- The collation and communication of key evidence
- The development of compelling narratives
- Engagement with and influencing of key decision makers
- Involvement in working groups to offer guidance and advice
A rapid expansion in the use and availability of technology and virtual solutions occurred during the COVID-19 pandemic. CPOC aims to build on benefits such as supporting patients in self-care, educating and training the workforce and the delivery of virtual consultations to facilitate and enhance perioperative care.
CPOC will signpost and support opportunities around artificial intelligence in prehabilitation and risk stratification, how information technology developments can improve patient flow, through improved multidisciplinary working and better communication and shared information.
We will promote better use of virtual technologies, such as remote monitoring, to support patient empowerment, offering a home-based approach to care.
We aim to:
- promote and support research and innovation for perioperative care.
- present, share and publish data on outcomes of perioperative care approaches
- support high quality research projects focussing on areas of importance to perioperative care
- support quality improvement programmes such as GIRFT,8 which highlight inconsistencies and variability in services provided across the UK.
To read more about the current work CPOC is undertaking, click here
If you have any ideas of workstreams you would like to propose under one of our strategic themes please visit our guideline proposal page.
Want to read the full strategy?